Voice care
See also free voice care literature and UK Voice Clinics directory
The Voice & Ageing
By Sara Harris, Speech and Language Therapist specialised in Voice Disorders.
How do we change with ageing?
Ageing is natural and affects us all. People’s voices do change with age, but the age at which these changes become noticeable is very variable, and many people weather ageing extremely well. The older voice is different from that of youth, but it also reflects the wisdom and rich experience of a lifetime.
Ageing and the body
Ageing changes occur throughout the body and may affect us in many ways. These general body changes can and do affect our voices adversely.
Joints and bones
Joints stiffen so that movement is restricted and often painful. The spine loses flexibility altering our posture. This can affect how the larynx is suspended from the skull and can also impact on free movement of the ribcage, making breathing more difficult.Bones become brittle and break more easily if we fall. Breaks in the arm, wrist or hip are particularly common as we get older and take longer to heal making it hard for us to get out and about, exercise and socialise.
Muscles
Muscles weaken and lose tone, becoming thin and stringy. We notice we have less stamina and are not as strong as we once were. This loss of muscle tone may directly affect the muscles in and around the voice box (the laryngeal muscles). It also contributes to changes in general body posture. Injuries or other medical conditions may mean long periods of inactivity, which also result in loss of muscle tone.Hearing
Our hearing deteriorates as we get older. From middle age many of us start to notice that we cannot make out what is being said against background noise. This is because the higher frequencies are lost, making sounds like “s” “sh” and “f” hard to discriminate.If hearing is more severely affected we may find it is hard to monitor the clarity of our speech. Certain sounds may be omitted or run together making us sound slurred or muffled.
Even if our own hearing survives well, that of our nearest and dearest may not. We may have to shout to make ourselves heard and this can irritate our voices making us hoarse.
Teeth
It is important to keep up regular dental checks. Our gums tend to recede with ageing and teeth may become loose and need removing. Missing teeth or dentures that do not fit well affect the articulation of speech, making it less clear.Breathing (the respiratory system)
The lungs lose capacity with ageing, making us more breathless. Our vocal folds rely on a steady air stream to vibrate them effectively, so speech may become effortful and we may notice we run out of breath before the ends of phrases.The digestive system
The digestive system slows down and is less efficient. Disorders such as diverticulitis and hiatus hernia are more common in older people causing abdominal pain or increasing the risk of acid reflux. Abdominal pain can affect the way we control breathing for speech or singing, while acid reflux can irritate the throat and gullet.Occasionally, acid from the stomach manages to spill over into the larynx causing violent coughing and irritation of the delicate membranes of the vocal folds and larynx. Even the threat of overspill is often enough to cause the larynx to rise and constrict in order to protect the airway.
The neurological system
The neurological input to our muscles changes with ageing. The overall number of nerves we have reduces and the spinal cord and brain shrink. The number of muscle motor pools is also reduced.A motor pool consists of all the motor nerves that serve (innervate) a single muscle. The motor nerves (neurones) are the nerves that carry electrical impulses from the brain to the muscles, preparing them for movement. Every muscle fibre is innervated by a motor neurone; however, each motor neurone may innervate several muscle fibres. As these diminish with age our fine movements, coordination and balance are likely to suffer.
This may affect swallowing, making it less coordinate so we are more likely to choke. Any food or drink that ‘goes the wrong way’ and gets into the larynx will cause paroxysmal coughing and irritation of the vocal folds.
It may also directly affect our speech in that movements of the tongue, palate and lips may slow down making speech less clear. We may also develop a tremor that affects the head, neck and voice as well as our limbs.
The brain
The brain also ages, causing it to shrink as it loses nerve cells. Most of us will notice some changes in our memories. We begin to forget things more easily, especially words and people’s names. While this is unlikely to affect our voices directly, these changes may affect our confidence in our ability to communicate easily with other. Conversation is a skill and we need to keep in practice!
Ageing and the voice
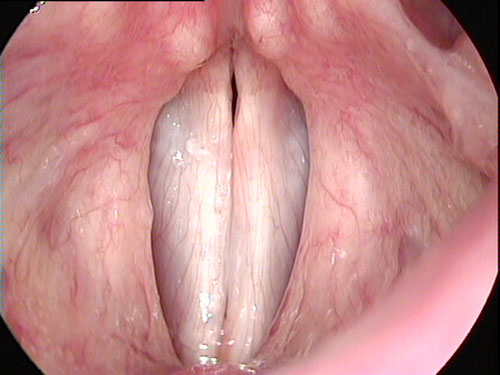
Normal vocal folds, closed (Photo: Tom Harris)
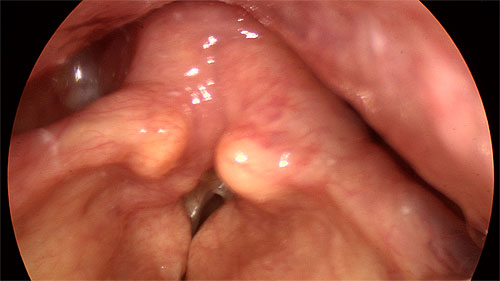
Bowing vocal folds with false fold recruitment (Photo: Nicholas Gibbins)
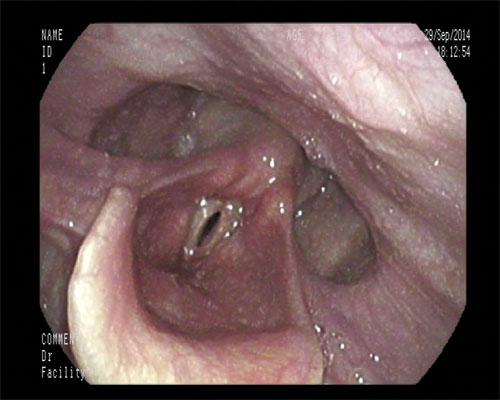
Bowing vocal folds in phonation (Photo: Nicholas Gibbins)
Our voices, as well as our bodies, alter over time. The most obvious change comes in boys at puberty when the larynx and vocal folds undergo a growth spurt. As the larynx grows, the vocal folds become longer and thicker and the pitch of the voice drops.
Both sexes are likely to notice some lowering of vocal pitch during middle age. Gravity causes the larynx to drop in the neck altering the distance from the vocal folds to the mouth (the vocal tract). The increase in vocal tract length alters its resonant features enhancing lower frequencies so the voice sounds lower.
Towards the end of middle age ageing changes begin to affect men and women differently. In women, the hormonal changes associated with menopause alter the vocal folds in a number of ways. They become stiffer and slightly thickened/swollen. The number of glands producing the mucus that lubricates them reduces, causing dryness, while the quality of the mucus alters becoming thicker and more difficult to clear. These vocal fold changes will significantly lower the pitch of the voice and the vocal quality will be rougher and breathier.
Men are more likely to notice that the vocal pitch rises after middle age. The vocal folds tend to lose their bulk becoming thinner and stiffer. They may lose their straight edges, so that when they close in the midline they no longer meet. A spindle-shaped gap develops between them, through which breath can escape, making the voice sound weak and breathy. This condition is usually referred to by doctors as “presbylarynx” “bowing vocal folds” or “glottic insufficiency”. Although presbylarynx is most common in elderly men, it can also occur in women in their later years.
Presbylarynx leads to a higher, often unstable vocal pitch that may yodel into falsetto. Occasionally two notes can be heard if falsetto and the normal lower voice are produced together (diplophonia). This instability of vocal pitch is most likely to occur when the volume/loudness is increased. The weak, breathy voice is harder to maintain and is physically effortful. Speaking is more tiring and may feel uncomfortable and strained. Changes in the neurological system may result in a tremor which will make the voice sound shaky, tight and strained.
The laryngeal cartilages calcify with ageing and the cricoarytenoid joints involved in opening and closing the vocal folds become stiffer. This may make it harder to close the vocal folds at the back (posteriorly), leaving a gap between the arytenoid cartilages through which breath can escape. Loss of fat and thinning of the vocal tissues may also cause a gap to develop at the front (anteriorly). This may also cause a breathier vocal quality and higher notes to ‘cut out’ in singing.
For most of us, these changes are gradual and never become severe enough to significantly affect our ability to communicate. Some people, however, are not so lucky. For them the deterioration associated with ageing occurs early and does impact on their communication and social activities. When this happens help is needed.
My voice has changed, what should I do?
Unfortunately many of the vocal changes associated with ageing also occur with other medical conditions. It is therefore important to eliminate any other cause before assuming any hoarseness/vocal change is due to ageing.
In order to do this you will need to see your GP and ask for a referral to an ENT surgeon or preferably a voice clinic. The general ENT surgeon can give you a general examination of ears, nose and throat, including the vocal cords. They can organise a hearing test and, if it is required, arrange for you to have a hearing aid. They can also refer you to your local speech and language therapist. However, he/she may not have access to the specialist equipment that is needed to see small vocal fold defects, such as scars, that may be altering the voice quality. The general ENT surgeon may not have a special interest in voice or be familiar with the ways in which voice production can cause hoarseness.
Voice clinics, on the other hand, are staffed by voice specialist ENT surgeons and speech and language therapists (SLT), and may have support from other related professionals, such as singing voice coaches or voice specialist osteopaths or physiotherapists. The clinic will have specialist equipment available to rule out the presence of any small or hidden vocal fold problems and the clinic team will be able to identify any ineffective patterns of voice use.
The multidisciplinary voice clinic has a holistic approach to diagnosis and usually offers longer appointments for new patient assessments. This makes it easier to identify patients with other contributing medical conditions such as neurological conditions, chest disease or gut problems. They can then be referred to the appropriate speciality for further assessment/treatment.
Treatment
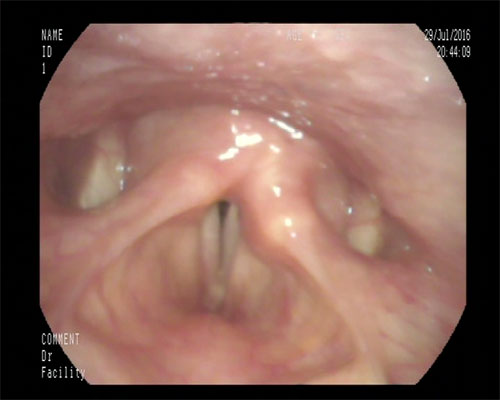
Glottic incompetance following injection adduction (Photo: Nicholas Gibbins)
Often vocal changes from ageing respond well to voice therapy. The voice clinic SLT will arrange this and monitor the outcome. In some cases of presbylarynx, voice therapy alone is not enough. The ENT surgeon may then offer surgical intervention. The vocal folds can be injected with fat (or some other medically appropriate filler) to increase their bulk so they are able to meet fully in the midline again. This is usually known as a ‘vocal fold augmentation injection’ or occasionally as a ‘voice lift’. The voice is usually lower and louder following the injection and the stamina improves but it may remain a little hoarse in quality.
What can we do to keep our voices good?
It is a case of ‘use it or lose it’. We need to exercise out voices just as we would any other muscle. This can be difficult for older people who may have few social contacts. They may need to be encouraged to keep using their voices and to find new ways to socialise.
We should all make the effort to see or telephone friends and relatives regularly and to talk to people in shops or on the bus when we are out. Even talking to the dog, the cat or yourself will help!
- Try starting the day with a vocal warm up (watch our 'Vocal warm-up' video on the 'Free Resources' page)
- Singing has been shown to be effective in keeping the voice working well and improving wellbeing. Consider taking lessons or joining a choir. You can search online to find choirs in your area, and many do not require you to read music or audition for a place. If you don’t have access to a computer, ask in the local library and the libra ian should be able to help you find one.
- Make sure you exercise regularly – this helps keep you stronger, more flexible and improves your breathing and posture. Walking, swimming and cycling are great ways to exercise, or join a local Tai Chi, Yoga or Pilates class.
- Make sure you eat a healthy and varied diet and try to keep your weight right for your height.
- Keep well hydrated – eight glasses of water a day is usually recommended in addition to any teas/coffees you may drink. It helps to cut down on caffeine, too.
- If you smoke, ask your GP for help to give up. Smoking is like taking sandpaper to your voice and puts you at higher risk of cancer of the lungs and airway.
- Keep alcohol to a minimum. It is irritating to the membranes of the mouth, throat, gullet and stomach. It may contribute to acid reflux and it also has an adverse effect on your brain and neurology.
- Keep mentally active. Reading the papers, doing crosswords, puzzles and games like Scrabble all help keep your mind active and your vocabulary from shrinking.
- Make sure your hearing has been checked and use your hearing aid if you have one. It helps you monitor your speech so the articulation stays clear. It is frustrating to have to say things twice!
Although we cannot stop the ravages of time, we can all improve our physical and vocal health by following the simple guidelines above and improving our lifestyles. We are likely to feel fitter and happier as a result.
With thanks to: Kristine Carroll-Porczynski, Jackie Ellis, Sophie Harris, Tom Harris and John Rubin for their editing skills and to Nick Gibbins and Tom Harris for the photographs.
Useful references:
- Cellular and Molecular Mechanics of Ageing of the Vocal Fold
Leslie T. Malmgren. In: Professional Voice: the art and science of clinical care. Volume 1: basic science and clinical assessment. Chapter 11: P 205: Ed. Robert Thayer Sataloff, Plural Publishing, 2005 - The Voice and Ageing
American Academy of Otolaryngology-Head and Neck Surgery. Patient Health Information at: www.entnet.org/content/voice-and-aging - The Effect of Music Therapy on Mood, Speech and Singing in People with Parkinson’s Disease – a feasibility study
Elefant C, Baker FA, Lotan M Lagesen SK, Skeie GO. Journal of Music Therapy, 49(3):278-302, 2012 - The Influence of Group Singing Therapy on the Behaviour of Alzheimer's Disease Patients
Kristine A. Olderog Millard and Jeffrey M. Smith J Music Therapy (1989) 26 (2): 58-70 - Cracking The Voice – what really happens when a singing voice gets old?
Justin Davidson, New York Magazine, October 6th 2016 (see also the hard copy edition of 2nd October 2016) - This is a Voice
Jeremy Fisher and Gillyanne Kayes. The Wellcome Collection, 2016, wellcomecollection.org - Vocal Warm up: Put Your Best Voice Forward
American Academy of Otolaryngology-Head and neck surgery. Patient health information at: www.entnet.org/content/vocal-warmup-put-your-best-voice-forward
This information is intended for guidance purposes only and is in no way intended to replace professional clinical advice by a qualified practitioner.

 Join us Now!
Join us Now! our newsletter
our newsletter free voice care leaflets & information – download here
free voice care leaflets & information – download here Help our work by donating while you shop
Help our work by donating while you shop