Voice care
See also free voice care literature and UK Voice Clinics directory
When it isn't just physical: The effects of stress and emotion on the voice
By Sara Harris, Speech and Language Therapist specialised in Voice Disorders. With grateful thanks and acknowledgements for comments, photographs and editing to: Tony Aymat, ENT Surgeon/Laryngologist, Peter Butcher, Consultant Psychologist, Annie Elias, Voice Specialist Speech and Language Therapist, Nick Gibbins, ENT Surgeon/Laryngologist, Tom Harris, ENT Surgeon/Laryngologist, John Rubin, ENT Surgeon/Laryngologist.
Voice disorders can affect your work and social life considerably, causing worry and frustration. The severity of the symptoms can vary enormously. Some people find they can barely whisper, while others can sound relatively normal but suffer pain and fatigue whenever they have to use their voices. Examination by an Ear Nose and Throat (ENT) Surgeon may well establish the presence of a disease or abnormality on the vocal folds that can explain the symptoms. However, often there are no signs of physical damage or disease and only small changes in the way the voice is produced are seen which cannot account for the severity of the voice loss.
It is often a shock to be told that nothing is physically wrong with the voice when the symptoms sound and feel severe to the patient. It can be hard to understand and believe, especially when the specialist explains that the voice problem is likely to be stress related.
So why does emotional stress affect our voices and how can this be treated?
What do we mean by stress?
When people talk about ‘stress’ we usually think of serious life events that upset us or make us angry or frightened. Examples would be bereavement, redundancy, serious illness, divorce, family disharmony or a violent assault. Even positive life events like moving house, having a baby or getting married are usually recognised as stressful but few of us ever see our routine, everyday lives as particularly problematic. However, if we look back over the last few months to a year or so, most of us will have had times when life has managed to get on top of us and we have felt down. It can be as simple as just a slow build up of pressure and work overload, when we feel we have too much to do in too little time. It is often these periods of unrecognised stress that begin to take their toll on our health and which can ultimately result in physical symptoms, such as a voice disorder.
When we are stressed we react both physically and emotionally. We may feel irritable, anxious or depressed, or we may notice physical changes such as increased muscle tension, headaches, difficulty sleeping or digestive problems. Often these symptoms come and go and we either ignore them or attribute them to other causes, such as fighting off an infection or eating something that disagreed with us. It is only when the symptoms become persistent or severe enough to worry us that we seek help.
How can emotional stress affect my voice?
The vocal tract which includes the larynx, (which houses the vocal folds/cords) and the pharynx (the area above the larynx often thought of as the throat) has a rich and complex nerve supply with input from both the Central Nervous System (CNS), which allows us voluntary control of movement for activities such as speaking or singing, and the Autonomic Nervous System (ANS), which regulates the function of our internal organs such as blood pressure, heart rate, swallowing, gut activity and digestion.
The ANS has three divisions, the parasympathetic, sympathetic and enteric systems. The parasympathetic system is our ‘rest and digest’ system, responsible for slowing heart rate, reducing blood pressure and increasing the digestive movements of the gut (peristalsis) when we are relaxed. It also increases the secretion of saliva and digestive juices.
The sympathetic nervous system is largely responsible for our ‘fight or flight’ response and prepares the body for action. It increases heart rate and blood pressure, reduces peristalsis and decreases the amount of saliva and mucus produced.
The enteric nervous system is a mesh of nerves that serve the intestines, pancreas and gall bladder.
The Autonomic Nervous System is closely linked with the emotion centres in the brain and this connection helps explain why, for example, we are able to recognise when our loved ones are upset or angry from subtle changes in facial expression, body posture and, of course, tone of voice.
When we perceive something as threatening or upsetting the body reacts rapidly, preparing for action and producing physical changes that we are all familiar with. These may include:
- Increased muscle tension
- Increased heart and breathing rates
- Perceived changes in temperature with shivering or sweating
- Tremor
- Dry mouth and throat
Emotions and their effects
Emotions are also experienced mentally and physically and our physical reactions to different emotions are often similar. Think how you feel when excited and when frightened; both emotions may result in increased muscle tension, tremor and palpitations but we interpret them differently. The physical symptoms experienced when excited, happy and engaged are perceived as a positive. They are motivating, energising and generally improve our performance. They are short term and we feel equal to the task we have taken on. In contrast, genuine fear or anger is perceived as unpleasant ‘distress’. Now the physical symptoms feel unpleasant, our performance is decreased and the task we have taken on may feel outside the range we can comfortably cope with.
Situations that produce distress may be short lived, such as a disagreement, or long term, such as illness or bereavement. However, distress can also be internally triggered by our habitual thoughts, associations and behaviour. For example, a bad experience with a dog as a child can set up a fear response that is triggered even when exposed to a friendly dog. Sometimes just the thought of a dog will be enough to set off our internal alarm system. Our behaviour may be affected in that we begin to avoid the park or places where we might come in contact with dogs.
Our habitual behaviour can create stressful situations too. We may tend to take on too much work, be unable to say ‘no’ or leave things until the last minute then pay the price by panicking. However it happens, when situations in our lives create emotional distress we find it difficult to deal with. We may choose to ignore the symptoms and signs and ‘get on with life’ but our bodies still react to the distress, developing physical symptoms. Common physical signs of distress include:
- Gut problems: (e.g. acid reflux and irritable bowel syndrome)
- Skin problems: (e.g. eczema /psoriasis)
- Back, neck or other muscle pain (including laryngeal pain)
- Breathing difficulties: (e.g. over-breathing panic attacks, a trigger for attacks in some asthmatics)
- Hoarseness (dysphonia) or complete voice loss/whisper (aphonia)
The symptoms are perfectly real but may be occurring in response to emotional distress rather than related to infection, physical abnormality or disease. Voice loss associated with emotional distress is usually termed a ‘psychogenic’ voice disorder. However, clinicians vary in their use of terms and other terms that may be used include ‘conversion’ aphonia/dysphonia, or occasionally ‘functional’ aphonia/dysphonia. The term ‘conversion’ is quite commonly used as, in essence, the emotional distress is literally being converted into a physical problem, in this case a disturbance of the voice. The individual adopts the voice disorder as a coping mechanism to deal with emotional distress but it is not a process under their voluntary control at the time. While most people with psychogenic dysphonia are aware they are stressed, others are not. Where they are unaware the diagnosis will come as a complete surprise and be hard to believe.
Symptoms of Psychogenic Dysphonia
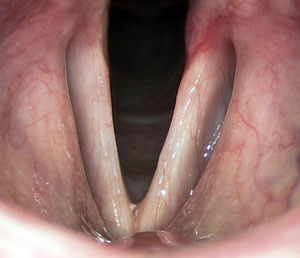
Normal vocal folds open in quiet breathing
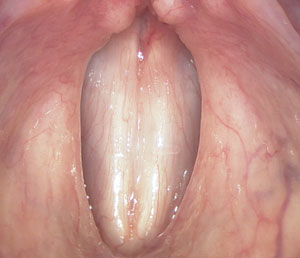
Normal vocal folds closed for voicing
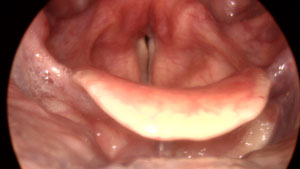
Vocal folds closed for voicing with lateral
compression and increased muscle tension
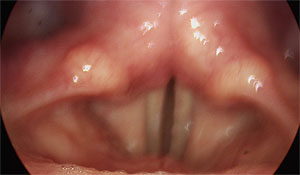
Vocal folds apart in phonation as for a whisper
Having a voice disorder in itself is extremely stressful and it is often difficult to tell whether the emotional factors are causative or a response to vocal fold damage, disease or overuse. There are, however, some signs that can be good indicators. For example, cases when the voice loss occurs suddenly and for no apparent reason. The person may have a normal voice one day then wake the next morning with only a whisper, although normal voice is often still heard in coughing or laughing. Recovery may be equally sudden with no apparent cause. Usually complete voice loss to a whisper (sometimes referred to as ‘whisper dysphonia’) will last for quite a while. Several weeks or months are characteristic but in other cases the voice may come and go over longer periods for months or even years. Other indicators include hoarseness initially associated with infection/overuse that fails to recover with time and the appropriate treatment, or persistent/excessive laryngeal pain in the absence of any laryngeal abnormality.
Diagnosis
Psychogenic voice disorders can affect adults and children, so if you, or your child, become hoarse or experience complete voice loss, the most important thing is to exclude any physical cause. You will need to see your GP, who will arrange a referral to an ENT surgeon or, better still, a voice clinic where there will also be a voice specialist Speech and Language Therapist (SLT) who can offer further assessment and treatment. Your GP can also diagnose and treat any other contributing medical conditions.
What can be done to help?
Speech and Language Therapy: SLTs are usually very effective at helping patients resolve psychogenic voice disorders. They have many useful vocal techniques and exercises that can recover the voice quickly and enable patients to cope again with their normal vocal workload. In addition, many SLTs are dual trained in counselling techniques and are able to work with patients to uncover the underlying emotional causes of the voice problem. They may introduce strategies to help patients learn to relax and look after themselves better, as well as helping them become more confident in expressing their feelings and learning to say what they want to say in difficult situations. Some are able to provide a limited number of counselling sessions to support patients as they improve the way they cope with emotional stress and work through their difficulties.
Counselling/Psychotherapy: Sometimes the emotional aspects need professional help from a Counsellor, Psychologist or Psychotherapist. There are many different psychological approaches available and it is important to find one that suits you. Often the popular conception of psychotherapy is that it focuses largely on the past and the unconscious. This approach is often called a ‘Psychodynamic’ approach with the most well recognised exponent being Sigmund Freud. Recently however, there has been a shift in focus towards solving difficulties in the present, developing effective coping strategies and challenging the habitual thoughts and behaviours that can cause difficulties in our relationships and work lives. Your GP will be able to help you find what is available in your area on the NHS (and maybe also privately). The various approaches are also relatively easy to research on the internet. It is very important that you choose a properly qualified therapist in whatever approach you choose. It is best to contact the appropriate professional body that regulates clinical practice and standards for help in seeking a private therapist (see reference section below).
One psychotherapy technique that has been used successfully with voice disorders is Cognitive Behavioural Therapy (CBT). This approach may be available on the NHS through your GP or by contacting the ‘Improving Access to Psychological Therapies’ (IAPT) scheme. Private CBT therapists can be found via the British Association for Behavioural and Cognitive Psychotherapy (BABCP) or through the British Association of Counselling and Psychotherapy (BACP) (see reference section below).
Manual Therapy/Laryngeal Massage: Muscle tension in and around the larynx can be a major component of psychogenic voice disorders making speaking effortful and painful. Sometimes this muscle tension is difficult to resolve with voice therapy alone. In cases such as these, laryngeal massage/manipulation can be useful. Some SLTs are trained in manual therapy techniques or these can be carried out by a Physiotherapist or Osteopath who specialises in voice disorders. Your SLT can usually help you find these services or you may be able to find them via their respective professional associations (see reference section).
Medication: Very occasionally psychogenic voice disorders fail to respond to speech therapy. There may be associated depression or some other psychological disorder that would respond better to medication. In this case, your GP will either help you find the most suitable medication or will refer you on to a Psychiatrist (a medical doctor specialising in mental health) for further assessment and help.
If your voice disorder is stress related there is no need to feel embarrassed or ashamed. It is often just your body’s way of letting you know there is a problem you need to attend to. The more we learn about how the mind and body interact together the more we realise that the mind can affect our health. So, if you develop a voice problem please seek help. Voice disorders usually respond very well to treatment and psychogenic based voice disorders often resolve quickly and completely.
Useful links
Psychotherapy
Improving Access to Psychological Therapy (IAPT): www.iapt.nhs.uk
The British Association for Behavioural and Cognitive Psychotherapy: www.babcp.com
British Association of Counselling and Psychotherapy (BACP) ‘Find a Therapist’ website at: www.itsgoodtotalk.org.uk
The British Psychodynamic Council: www.bpc.org.uk/find-a-therapist
Manual Therapy
The Institute of Osteopathy: www.osteopathy.org
The Chartered Society of Physiotherapy: www.csp.org.uk
Speech and Language Therapy
The Royal College of Speech and Language Therapists: www.rcslt.org
Health and Care and Professions Council: www.hpc-uk.org
This information is intended for guidance purposes only and is in no way intended to replace professional clinical advice by a qualified practitioner.

 Join us Now!
Join us Now! our newsletter
our newsletter free voice care leaflets & information – download here
free voice care leaflets & information – download here Help our work by donating while you shop
Help our work by donating while you shop